Volume Modes - Assist-Control Ventilation (ACV)
- Synchronized Intermittent-Mandatory Ventilation (SIMV)
- ACV vs.
- Pressure-Controlled Ventilation (PCV)
- Pressure Support Ventilation (PSV)
- Pressure Controlled Inverse Ratio Ventilation (PCIRV)
- Airway Pressure Release Ventilation (APRV)
- Pressure Regulated Volume Control (PRVC)
.
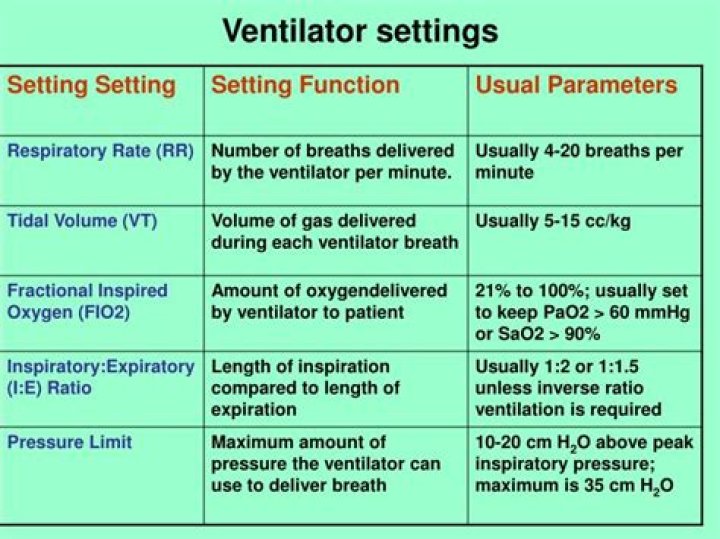
Just so, what are normal vent settings?
Initial Adult Ventilator Settings. You have to start somewhere ✓ Fraction of inspired oxygen (FiO2)—100% ✓ Positive End Expiratory Pressure (PEEP)–5 cmH20 ✓ Respiratory Rate—12 breaths per minute ✓ Tidal Volume 6-8 ml per weight in kilograms (ideal body weight). Most adults will require at least 500 ml.
Beside above, what does peep stand for? positive end-expiratory pressure
Likewise, people ask, what are the different modes of ventilation?
Based on the types of respiratory cycles that are offered to the patient, three basic ventilatory modes can be considered. These are: Assist/Control ventilation (A/C), Pressure Support Ventilation (PSV) and Synchronized Intermittent Mandatory Ventilation (SIMV) with PS, a hybrid mode of the first two.
Why is auto peep bad?
Dynamic hyperinflation with intrinsic expiratory flow obstruction is the most common cause of auto-PEEP in COPD patients in whom alveolar collapse during expiration leads to air trapping.
Related Question Answers
What is PIP ventilator setting?
Peak inspiratory pressure (PIP) is the highest level of pressure applied to the lungs during inhalation. Peak inspiratory pressure increases with any airway resistance. Things that may increase PIP could be increased secretions, bronchospasm, biting down on ventilation tubing, and decreased lung compliance.What is ventilator in ICU?
Use of a ventilator is also commonly referred to as "life support" or life sustaining equipment. This means that without the machine the patient would not survive. A ventilator is a type of equipment that is used in the ICU to assist people in breathing when they are unable to do so themselves.What is the definition of tidal volume?
Tidal volume (symbol VT or TV) is the lung volume representing the normal volume of air displaced between normal inhalation and exhalation when extra effort is not applied. In a healthy, young human adult, tidal volume is approximately 500 mL per inspiration or 7 mL/kg of body mass.What is Simv mode?
Synchronized Intermittend Mandatoryl Ventilation (SIMV) describes a method of providing mechanical breaths to a patient. In the SIMV mode, the patient is allowed to take additional breaths in between the mechanical breaths. The patient's own breaths are called "spontaneous breaths".Can a person die on a ventilator?
People tend to stop breathing and die soon after a ventilator shuts off, though some do start breathing again on their own. If he is not taking in any fluids, he will usually die within several days of a feeding tube removal, though he may survive for as long as a week or two.What is the difference between oxygenation and ventilation?
Ventilation and oxygenation are distinct but interdependent physiological processes. While ventilation can be thought of as the delivery system that presents oxygen-rich air to the alveoli, oxygenation is the process of delivering O2 from the alveoli to the tissues in order to maintain cellular activity.What are the two types of ventilation?
There are two basic types of natural ventilation effects: buoyancy and wind. Buoyancy ventilation is more commonly referred to as temperature-induced or stack ventilation.How does peep work?
Positive end expiratory pressure (PEEP), is a pressure applied by the ventilator at the end of each breath to ensure that the alveoli are not so prone to collapse. So PEEP: Reduces trauma to the alveoli. Improves oxygenation by 'recruiting' otherwise closed alveoli, thereby increasing the surface area for gas exchange.What is CPAP mode on ventilator?
? CPAP (Continuous Positive Airway Pressure) this mode of ventilation uses pressure. support and peep to allow the patient to spontaneously breathe on his own without any mechanical breaths being given. ? If a patient in this mode can maintain his. own respiratory effort without excess work, if.What is the difference between volume and pressure ventilation?
In summary: In general, volume control favours the control of ventilation, and pressure control favours the control of oxygenation. Volume and pressure control modes have distinct advantages and disadvantages which are mainly related to the flow and pressure patterns of gas delivery.What is the difference between IMV and Simv?
When IMV is synchronized to the patient's inspiratory efforts, it is referred to as synchronized IMV (SIMV) (Figure 49-11). In SIMV, the total number of mandatory breaths will only be equal to the preset frequency of mandatory breaths. SIMV breaths can be both volume regulated or pressure limited.What is ventilation in the body?
Medical Definition of Ventilation Ventilation: The exchange of air between the lungs and the atmosphere so that oxygen can be exchanged for carbon dioxide in the alveoli (the tiny air sacs in the lungs).How do you measure tidal volume?
Tidal volume is measured using several techniques and at several sites in the breathing circuit. Common measures include the setting on the ventilator control panel, bellows excursion, and flow through the inspiratory or expiratory limbs of the circuit.What is AC ventilation mode?
Assist-Control (AC) mode is one of the most common methods of mechanical ventilation in the intensive care unit[2]. AC ventilation is a volume-cycled mode of ventilation. It works by setting a fixed tidal Volume (VT) that the ventilator will deliver at set intervals of time or when the patient initiates a breath.What is P mean in ventilator?
From Wikipedia, the free encyclopedia. Mean airway pressure typically refers to the mean pressure applied during positive-pressure mechanical ventilation. Mean airway pressure correlates with alveolar ventilation, arterial oxygenation, hemodynamic performance, and barotrauma.How do ventilation systems work?
Exhaust ventilation systems work by depressurizing the building. By reducing the inside air pressure below the outdoor air pressure, they extract indoor air from a house while make- up air infiltrates through leaks in the building shell and through intentional, passive vents.How serious is being on a ventilator?
One of the most serious and common risks of being on a ventilator is pneumonia. The breathing tube that's put in your airway can allow bacteria to enter your lungs. As a result, you may develop ventilator-associated pneumonia (VAP). Coughing helps clear your airways of lung irritants that can cause infections.What is intubation used for?
Intubation is the process of inserting a tube, called an endotracheal tube (ET), through the mouth and then into the airway. This is done so that a patient can be placed on a ventilator to assist with breathing during anesthesia, sedation, or severe illness.How do you adjust minute ventilation?
Alveoli. Minute ventilation is the tidal volume times the respiratory rate, usually, 500 mL × 12 breaths/min = 6000 mL/min. Increasing respiratory rate or tidal volume will increase minute ventilation.